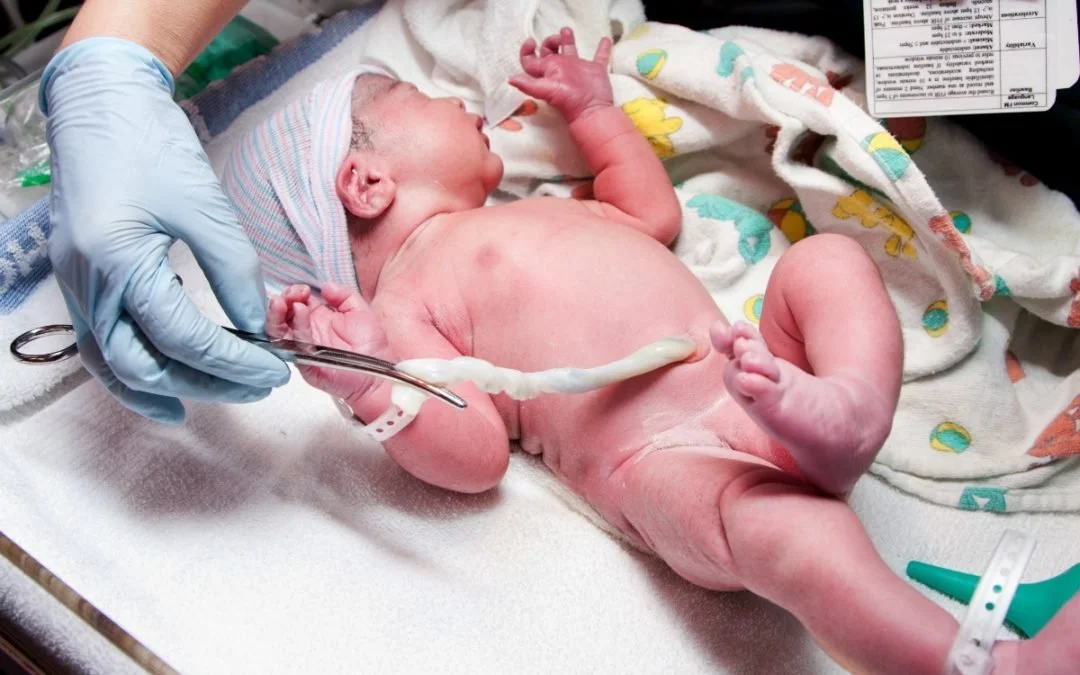
Delayed Cord Clamping: Why 60 Seconds May Not Be Enough (A Doula / Birth Keeper Perspective)
If you’re pregnant — or thinking about becoming pregnant — you’ve probably heard the term delayed cord clamping. But what does it actually mean, and why does it matter for your baby?
In many hospitals, “delayed” cord clamping often means waiting 30 to 60 seconds before clamping and cutting the umbilical cord. Sixty seconds.
That sounds reasonable… until you understand what’s happening in your baby’s body during that first minute.
This post is about giving you the information so you can participate in your birth, ask the right questions, and make decisions that align with your values. It’s about informed consent, not following routine protocol.
What Is Delayed Cord Clamping — Really?
Delayed cord clamping is simply waiting to clamp and cut the cord so blood can continue transferring from the placenta to your baby. This process is called placental transfusion.
At birth, about one-third of your baby’s blood volume is still in the placenta. That blood belongs to them — not your provider, not the hospital routine. It supports:
Circulation
Oxygen delivery
Iron stores
Organ perfusion
Cardiovascular transition
Full placental transfusion usually isn’t complete at 60 seconds. In many births, the cord continues pulsing for several minutes. This is why timing it by the clock alone can be limiting.
Why Blood Volume Matters for Newborn Transition
Newborn transition is a process, not a switch.
Babies can take up to five deep breaths to fully clear fluid from their lungs. Those first breaths are effortful and transitional. During that time, oxygen is still being supplied by the blood coming from the placenta.
Breathing supports circulation. Circulation delivers oxygen to the organs. Organs require oxygen to function well.
Blood volume affects perfusion — how effectively blood reaches tissues. And here’s a key point from Professor Stuart B. Hooper, a leading researcher in neonatal physiology:
“The heart can only pump the blood it receives, so delaying cord clamping until a baby is breathing is simply a matter of sustaining the input to the pump. It allows the input to immediately switch from the placenta to the lung when the cord is cut because the lungs are already aerated.”
In other words, delayed cord clamping isn’t just a policy or a tradition. It’s about supporting the baby’s heart and lungs during a critical transition. If the cord is clamped too early, we may interrupt that transition rather than supporting it.
One presentation I reviewed noted that if a newborn does not receive their full blood volume — roughly 80–100 mL — that deficit is physiologically comparable to an adult experiencing a major hemorrhage, losing 1,500–2,000 mL of blood.
Once you see the numbers, sixty seconds starts to feel very small.
What About Emergency Situations?
A common concern is: What if my baby needs resuscitation?
Most babies do not need resuscitation. Birth is designed to work. Most newborns transition on their own — otherwise we wouldn’t exist as a species.
Even in many resuscitation scenarios, emergency practices may support:
Bedside ventilation with the cord intact
Cord milking (when appropriate), sometimes up to four times before clamping
The baby should be assessed by breathing, tone, and color — not by a stopwatch.
We need to watch the baby. Not the clock.
Hospital Birth vs Home Birth: A Real Difference
In my work as a doula and birth keeper, I see a stark difference between how third stage is treated in hospital versus home birth settings.
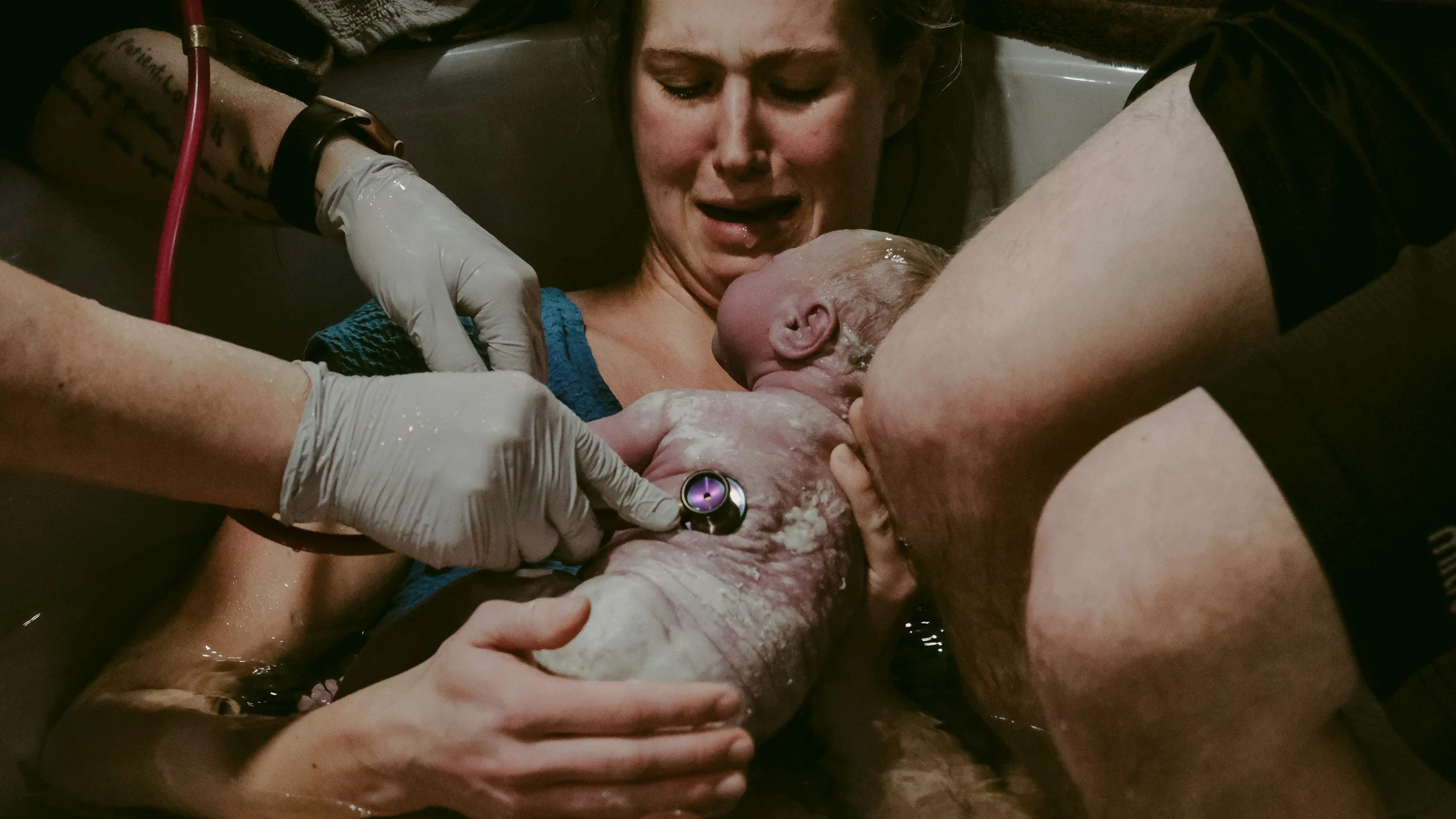
At home, physiology is often centered. Families are encouraged to have a bowl ready for the placenta. If birth happens in water, the placenta can remain beside the parent and baby while they rest and integrate.
I recently had someone share that she birthed in water and simply wasn’t ready to separate. She kept the placenta in a bowl floating beside them, and only cut the cord when she felt ready.
There was no rush. The baby was assessed by how they were doing, not by a clock.
In hospitals, policies, workflow pressures, equipment setup, and culture can mean that cords are clamped before full placental transfusion is complete. It’s not wrong — it’s the system — but it’s important for families to understand why it’s done this way so they can actively participate in their decisions about when to separate mom and baby via cord clamping and cutting.
How Long Should You Delay Cord Clamping?
Research supports at least 60 seconds (because that’s what the care providers do). However, it’s also common knowledge (even in hospitals) that waiting for the cord to stop pulsing, which may be 3–5 minutes — sometimes longer, is preferred for better APGAR scores.
Active management of the third stage, meaning when you’re giving birth to your placenta, is typically not considered prolonged until 20–30 minutes in most clinical settings. In most uncomplicated births, there is time.
The question isn’t “What is the standard?” The question is:
What feels aligned for you, once you understand the physiology and the options?
Because it is always up to you.
Questions to Ask Your Care Provider About Delayed Cord Clamping
If this is important to you, have a conversation before labor. Ask:
How long do you typically wait before clamping?
Under what circumstances would you recommend clamping sooner?
Can newborn resuscitation happen at the bedside with the cord intact?
Are you comfortable waiting until the cord stops pulsing?
What is your approach to placenta delivery / managing the third stage?
Asking these questions is not being difficult. It’s being informed.
Why Doula / Birth Keeper Support Matters
The first minutes after birth are intense. You’ll be meeting your baby. Your nervous system will be shifting. Your partner will likely be emotional and focused on you and the baby.
Cord clamping can happen quickly.
A doula or birth keeper cannot override medical decisions, but she can:
Track the moment calmly
Help you and your partner use your voice and remind the team of your preferences
Remind you to ask clarifying questions
Support bedside assessment to see if the cord has stopped pulsing
Help you navigate hospital dynamics in real time
Support logistics like getting your placenta bowl, helping you in and out of positions or space to transition into delivering your placenta, or assisting your partner, family members, friends, chosen family etc. in these steps
Having this support helps ensure your informed choice is honored — even in a busy or high-pressure birth environment.
Final Thoughts
Delayed cord clamping is not about rejecting medical care.
It’s about helping your baby THRIVE, not just the status quo.
It is about understanding physiology.
It is about supporting perfusion and oxygenation.
It is about allowing transition rather than interrupting it.
And it is always up to you.
If you are planning a your birth and want to create a clear strategy around delayed cord clamping and third stage management, this is something we can prepare for together in a focused consultation.
If you’re looking for doula / birth keeper support and want someone by your side who understands both physiology and hospital systems, reach out to connect.
You deserve to understand your options.
And your baby deserves a fully supported transition.
Additional Resources / Read More
Expert Insight:
“The heart can only pump the blood it receives, so delaying cord clamping until a baby is breathing is simply a matter of sustaining the input to the pump. It allows the input to immediately switch from the placenta to the lung when the cord is cut because the lungs are already aerated.” — Professor Stuart B. Hooper (Medical Xpress)
Research Resource:
• Hooper SB, Binder‑Heschl C, Polglase GR, et al. The timing of umbilical cord clamping at birth: physiological considerations. Maternal Health, Neonatology & Perinatology (2016). (Read full paper)
Disclaimer: This information is provided for educational purposes only and is not medical advice. Always discuss your individual circumstances, birth plan, and care options with your qualified healthcare provider.